The human anatomy is a remarkably advanced early warning mechanism, designed to emit intricate signals when its internal chemistry faces a fundamental crisis. One of the most perilous errors an individual can make is dismissively treating these signals as minor irritations. In the field of emergency care, few things are as misleading as a dermatological reaction. We are conditioned to view crimson spots, bumps, or itching as bothersome but ultimately benign issues that will fade with time or a basic topical cream. However, as we move through 2026, medical experts are issuing a stern caution: when specific skin symptoms manifest alongside even a minor change in your breathing, you are not facing a simple rash—you are facing a systemic biological emergency that could become fatal within minutes.
The Anatomy of an Emergency
The primary risk lies in how quietly these reactions can begin. Many people assume a sudden eruption of red patches is merely a temporary response to a new detergent or an environmental irritant. In reality, when the skin reacts at the same time the respiratory system begins to fail, the body is likely undergoing anaphylaxis. This is a severe, multi-system allergic response where the immune system releases a flood of chemicals that can trigger shock. In this scenario, the skin acts as the visible alarm for an invisible, life-threatening internal collapse.
Current data from 2024 to 2026 highlights significant disparities in how these conditions impact different populations in the United States:
- Prevalence: Diagnosed food allergies, a major trigger for anaphylaxis, are most prevalent in non-Hispanic Black adults at 9.9%, compared to White (6.4%), Asian (5.5%), and Hispanic (5.4%) adults.
- Pediatric Risk: Approximately 7.6% of non-Hispanic Black children have food allergies, and they are two to three times more likely than White children to suffer a fatal allergic reaction to food.
- Emergency Care: Black and Hispanic children are twice as likely as White children to experience a severe food allergy reaction or require an emergency department visit.
- Skin Manifestations: Allergic skin symptoms are most common in children who are Black (18.2%) or of multiple races (17.2%).
Recognizing the Critical Signs
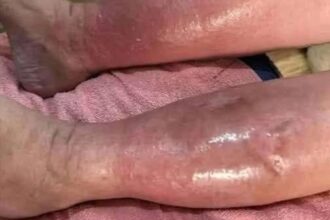
The raised, swollen red welts associated with these reactions are medically termed urticaria, or hives. These are not standard dry skin patches; they appear as irregular pinkish or red welts that can burn, itch, and spread with alarming speed. While hives alone can be manageable, their sudden appearance becomes a herald of disaster when the throat begins to constrict. In a systemic reaction, the same inflammation causing the welts on your arm is occurring within your airways, swelling the tissue and restricting oxygen flow.
The transition from irritation to emergency is marked by the “red line” of breathing difficulty. Experts urge hyper-awareness of these secondary signs:
- Shortness of breath or wheezing: Indicators that the airway is narrowing.
- Angioedema: Swelling of the lips, tongue, or face.
- Shock Indicators: A racing heart, dizziness, or a feeling of impending faintness.
Triggers and Immediate Action
The triggers for such a violent response are vast. For some, it is a known allergy to peanuts, shellfish, or eggs. For others, it could be a sudden reaction to a new medication, such as an antibiotic, or an insect sting. Frighteningly, these reactions can occur in individuals with no prior history of allergies; a person may use a product for decades without issue before their immune system suddenly identifies it as a mortal threat.
When hives and breathing difficulty collide, immediate action is the only variable that matters:
- Call Emergency Services: Do not wait to see if the symptoms pass.
- Administer Epinephrine: Use an auto-injector (like an EpiPen) immediately if available. Epinephrine works rapidly to constrict blood vessels and relax lung muscles.
- Stabilize the Patient: Keep the person lying down to stabilize blood pressure, unless this makes breathing more difficult.
In 2026, the takeaway remains clear: early recognition is the ultimate life-saving tool. While not every rash is a tragedy, the combination of skin changes and respiratory distress must always be treated as a maximum-level emergency. It is far better to seek evaluation for a minor reaction than to wait a single second too long when the body is signaling a systemic storm. Recognition is power, and in these critical moments, that power is exactly what saves lives.