The progress of cancer treatment is often measured in small steps—slightly longer survival times or slower tumor growth. But occasionally a development emerges that challenges expectations about what medicine might achieve.
In early 2024, researchers at Mass General Brigham launched a small clinical trial testing a new type of immunotherapy against Glioblastoma—one of the most difficult cancers to treat.
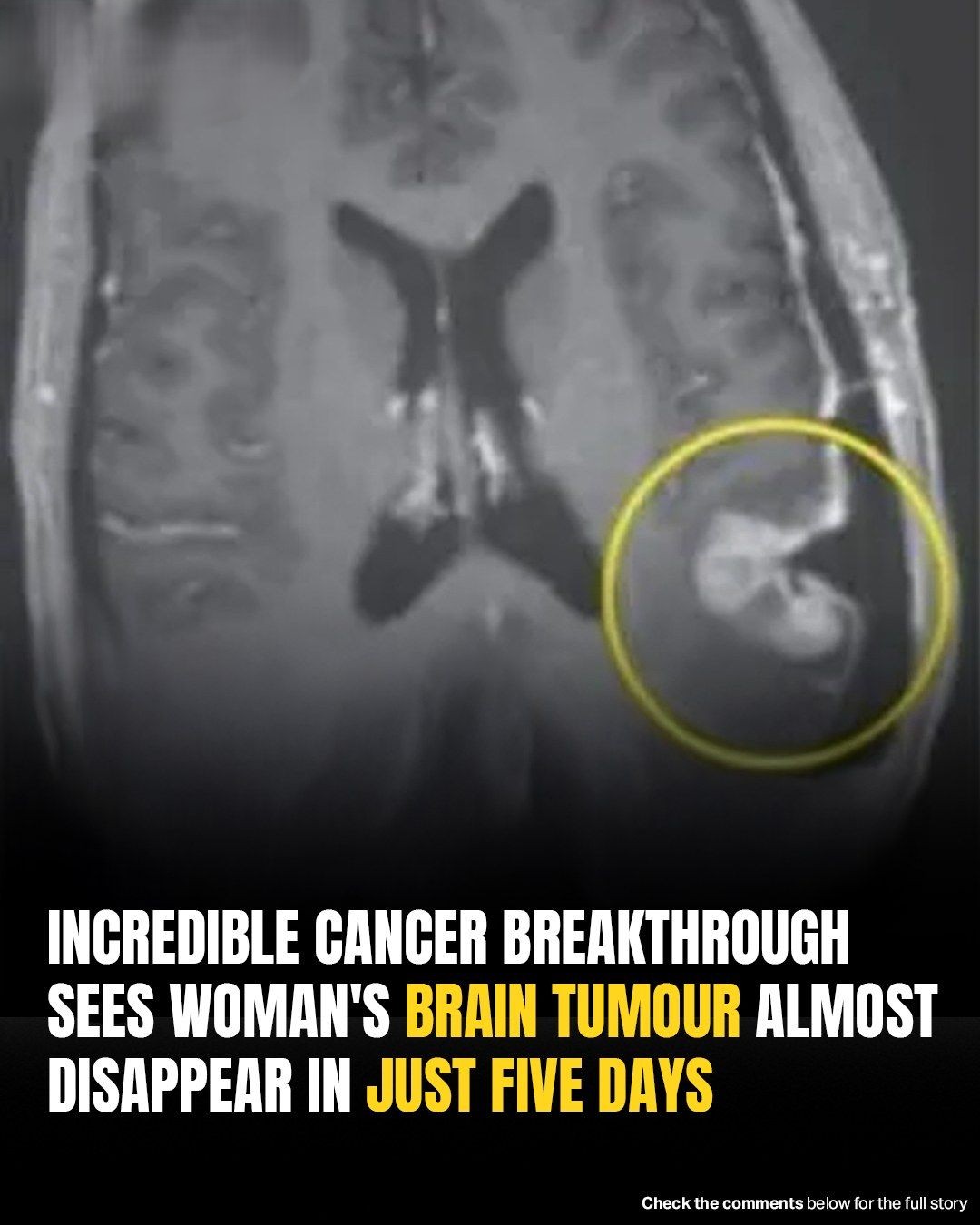
In one case from the trial, a patient with an inoperable brain tumor saw dramatic tumor shrinkage within days.
Why Glioblastoma Is So Difficult to Treat
Glioblastoma is widely considered one of the most aggressive brain cancers. Unlike many tumors that form clearly defined masses, glioblastoma spreads microscopic strands of cancer cells throughout healthy brain tissue.
This makes surgery extremely difficult because removing the entire tumor without damaging critical brain functions is often impossible.
Treatment is further complicated by the blood–brain barrier, a protective system that prevents many drugs from entering brain tissue. Because of this barrier, traditional chemotherapy often struggles to reach the tumor effectively.
Standard treatment usually involves surgery, radiation therapy, and chemotherapy with drugs such as temozolomide, but recurrence is extremely common.
The New Approach: Advanced CAR-T Immunotherapy
The research team used an experimental form of CAR-T cell therapy.
CAR-T therapy works by:
- Collecting a patient’s immune T-cells
- Genetically modifying them in a laboratory
- Programming them to recognize proteins on cancer cells
- Infusing them back into the patient so they can hunt down the tumor
This method has already shown major success in blood cancers such as leukemia and lymphoma. However, applying it to solid tumors like brain cancer has historically been much more difficult.
A Dual-Target Strategy
One reason CAR-T therapies struggle against solid tumors is tumor diversity. Glioblastoma cells often differ from one another, meaning some cells may escape treatments designed to target only one specific marker.
To address this problem, researchers combined CAR-T cells with specialized T-cell engaging antibody molecules, creating a multi-target immune response designed to recognize more than one tumor marker at the same time.
This approach helps prevent cancer cells from escaping the therapy by simply changing their surface proteins.
Delivering the Treatment Directly to the Brain
Instead of delivering the therapy through a standard intravenous infusion, doctors used an implanted device called an Ommaya reservoir.
This small device sits beneath the scalp and allows medication to be delivered directly into the cerebrospinal fluid surrounding the brain and spinal cord.
By bypassing the blood–brain barrier, the engineered immune cells can reach the tumor more efficiently.
Rapid Tumor Shrinkage Observed
The early trial involved three patients whose glioblastoma had returned after standard treatments.
Researchers observed unusually rapid responses:
- One patient experienced measurable tumor shrinkage within 48 hours
- Another patient’s tumor dramatically regressed within five days
- A third patient showed similar early improvement on MRI scans
For a cancer known for resisting treatment, the speed of these responses surprised many specialists.
Early Results, But Promising
Despite the dramatic early changes, scientists emphasize that the findings are preliminary. The study was a Phase 1 trial, designed mainly to evaluate safety rather than long-term effectiveness.
Researchers are continuing to monitor:
- How long the tumor responses last
- Potential side effects, including brain inflammation
- Whether similar results can occur in larger groups of patients
The brain is an extremely sensitive organ, and strong immune reactions can sometimes cause swelling or neurological complications.
What This Could Mean for Future Cancer Treatments
Even though it is still early, the study offers an important proof of concept: with the right engineering and delivery method, the immune system can attack even highly resistant brain tumors.
If future trials confirm the results, this strategy could open the door to new treatments for cancers that have historically had very few options.
For patients and families facing glioblastoma, developments like this provide cautious but meaningful hope that more effective therapies may be on the horizon.