The human body is an intricate map of biological indicators, where every freckle, line, and vessel can seem like a coded message about our internal health. Among the most common points of curiosity—and occasionally, anxiety—is the appearance of the hands. For many, a sudden realization that the veins on the back of the hand have become raised, bluish, or more pronounced leads to a flurry of digital self-diagnosis. One of the more persistent myths circulating in online wellness spaces is the idea that prominent hand veins are a “silent” warning sign of kidney disease. However, when we hold this theory up to the light of clinical nephrology and vascular biology, the connection dissolves, revealing a much more benign reality rooted in anatomy, aging, and hydration.
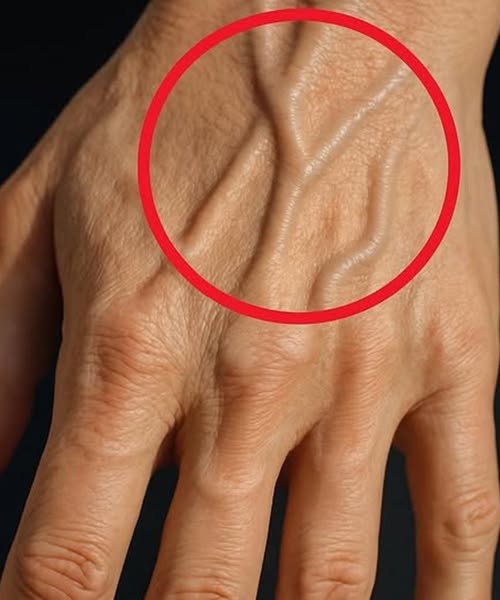
To understand why veins become prominent, we must first understand the architecture of the hand. Unlike the deep veins tucked away near the bone, the veins on the back of the hand are superficial. They sit just beneath the dermis in a layer of subcutaneous fat. Consequently, the visibility of these vessels is less about the health of the blood itself and more about the “canvas” covering them. There are several physiological reasons why these veins might suddenly appear to “pop,” almost none of which involve the renal system.+2
The most common factor is the natural process of aging. As we move through the decades, our skin undergoes structural changes; it loses elasticity and, more crucially, it thins. The production of collagen and elastin slows down, and the protective layer of subcutaneous fat begins to dissipate. With less “padding” and a thinner exterior, the underlying vascular structures become much more apparent. This is a normal anatomical progression, not a pathological one. Similarly, individuals with low body fat percentages or high muscle definition often have very visible veins because there is simply less tissue to obscure them. This is why athletes often display high levels of vascularity; their bodies are efficient machines with minimal insulation between the muscle and the skin.+1
Environmental and lifestyle factors also play a significant role. Heat exposure is a primary culprit; when the body becomes warm, the veins dilate (a process called vasodilation) to help move blood closer to the skin’s surface, allowing heat to escape and the body to cool down. Physical activity has a similar effect, as the heart pumps more blood to the extremities to support movement. Even hydration levels fluctuate the visibility of these vessels. Interestingly, mild dehydration can actually make veins look more prominent as the surrounding skin loses turgor and clings more tightly to the underlying structures.
When we pivot to the actual clinical presentation of kidney disease, the “visible vein” theory becomes even more contradictory. The kidneys are the body’s master regulators of fluid balance, blood pressure, and electrolyte filtration. When the kidneys begin to fail—as seen in Chronic Kidney Disease (CKD)—the body does not typically lose fluid volume in a way that would make veins prominent. Instead, it does the opposite: it retains fluid. This pathological fluid retention, known as edema, causes the tissues to swell. In a patient with significant kidney dysfunction, the hands and feet often become puffy and “pitting.” This extra fluid creates more distance between the skin and the veins, which actually makes the veins less visible, not more.+2
The true warning signs of kidney distress are systemic and measurable, rather than purely aesthetic. Nephrologists look for a specific cluster of symptoms that indicate the filtration system is struggling. These include persistent fatigue caused by anemia (the kidneys produce a hormone that signals red blood cell production), changes in the frequency or color of urination, and foamy urine, which indicates that protein—something the body should keep—is leaking through damaged filters. High blood pressure that is difficult to control is another hallmark, as the kidneys play a vital role in regulating the hormones that constrict or relax blood vessels.+1
There is, however, one specific intersection where kidney disease and visible veins meet, but it is a result of treatment rather than a symptom of the illness itself. In patients with end-stage renal disease who require hemodialysis, surgeons often create an arteriovenous (AV) fistula. This procedure surgically connects an artery directly to a vein, usually in the arm or hand. The high-pressure arterial blood flows into the vein, causing it to grow significantly thicker and stronger so it can withstand the large needles used for dialysis. In these cases, a patient will have a very prominent, ropelike vein, but this is an intentional medical intervention designed to save their life, not a natural symptom of the disease’s onset.
The danger of focusing on “hand veins” as a diagnostic tool is that it can lead to unnecessary panic while distracting from the markers that truly matter. Kidney disease is often called a “silent killer” because its early stages frequently produce no symptoms at all. By the time a person feels “sick,” the damage may be advanced. Therefore, the gold standard for kidney health is not a visual inspection of the hands, but a series of simple clinical tests. A blood test to check creatinine levels and the Estimated Glomerular Filtration Rate (eGFR) provides a mathematical window into how well the kidneys are cleaning the blood. A urine test can check for albumin (protein), which is the “canary in the coal mine” for kidney damage.+2
If you notice your hand veins are becoming more visible, the most likely explanations are that you are staying active, you have a lean physique, or you are experiencing the natural, graceful thinning of the skin that comes with a life well-lived. If the veins are accompanied by pain, redness, or warmth, the issue is likely vascular—perhaps a localized inflammation or a clot—rather than renal.
Ultimately, our hands tell the story of our lives: the work we’ve done, the temperatures we’ve endured, and the years we’ve gathered. While they are excellent tools for interaction, they are not a reliable dashboard for kidney function. Protecting your kidneys involves maintaining a healthy blood pressure, managing blood sugar, staying properly hydrated, and getting regular check-ups. Trust the science of the laboratory over the myths of the internet. If your lab results are healthy, you can view those prominent veins not as a sign of hidden illness, but as a sign of a body that is effectively circulating the lifeblood that keeps you moving every day.